“Stand up straight and realize who you are, that you tower over your circumstances. You are a child of God. Stand up straight.” ~Maya Angelou
These words saved me today. When I felt myself start to crumble, instead I stood a little straighter. Now is not the time. There is work to be done.
Benjamin’s fever broke last night and his pulse slowed to a high but acceptable rate. We both got choppy sleep. I was awake at shift change to see lab numbers that were consistent with Saturday’s results; white count of 6,670, 81% blasts, zero immunity, blood and platelet transfusions needed today. Benjamin was softly moaning through the report. I joined him back in bed, and we slept soundly for the next three hours.
When we woke for the day, I learned that Benji’s electrolytes were off, his calcium and sodium were low, and his creatinine was high. Most importantly his albumen was low, an indicator that he isn’t absorbing enough protein. Without enough protein, his veins can’t retain the fluid they need. It partially explains his excess of fluid and need for lasix. The hydration isn’t going where it needs to go. The team’s solution was something we’ve been putting off as long as possible: total parenteral nutrition (TPN) through his port. It will correct all of these problems and ease the pressure on his kidneys, but it could be hard on his liver, and possibly increase his infection risk. It’s a move we have to make.
While Benjamin is on the TPN he will continue to get a smaller volume of formula through his feeding tube to keep his gut stimulated. The dietician told me he’d located a small supply of Liquid Hope for Benjamin while we wait for my order to arrive (I think our nurse practitioner may have had a little something to do with this). We made the switch today. It’s a small change but it made me feel so much better to be giving him quality nutrition. He hasn’t eaten a meal in two weeks.
I know Benjamin heard me telling the nurses that when he sat upright in the chair last night, he didn’t need oxygen. That’s why he asked to sit in the chair again this morning. He tries so hard to do the right thing. I pulled a chair next to the bed, and he sat, and drank water, and looked out the window while I changed his linens. I can’t really express how happy I was to see him with sunshine on his face.
Benji was exhausted from his efforts. He pushed his pain button twice when he got back into bed. He was very uncomfortable. Dr. Wishnew is the attending physician this week; she came in with Shari, our nurse practitioner, on rounds. They stayed in our room for a really long time, just watching Benjamin’s labored breathing. The silence in the room was so thick I felt like I would suffocate. Finally, as we were talking about the logistics of Benji’s medicines, Dr. Wishnew asked me how I was doing. I told her I was just ready to get Benji to Maryland. She looked me in the eye and said, “I’m worried about him. He’s really sick. I’m worried there isn’t enough time.”
My stomach. Dr. Wishnew didn’t say anything I didn’t know. Everyone is worried about the timeline here. Everyone is worried about Benjamin’s organs. But the words had not been said, until they were, and then they hung in the air forever, suspended by my own disbelief.
As soon as Dr. Wishnew and Shari left the room, I felt myself begin to dissolve. Not now. No fear. No giving up. I am present for Benjamin. I stood up straighter. I texted Michael to make sure we were on the same page with the email to Dr. Oshrine. I made a few changes to yesterday’s draft and hit send. When Michael called me on his way over the bridge, the sound of his voice went straight into my chest.
Benjamin’s moaning sometimes sounds like labor pain, and sometimes it’s almost humming, melodic. The pain team heard these sounds. We agreed to increase the dose of Benjamin’s Fentanyl patch once more, and to add a patch of Clonidine to help him relax. He is also now on a low dose of Narcan to relieve the itching caused by his pain medicines. His IV pole has three central pumps and so many bags hanging on it now I’m surprised it doesn’t topple over.
The palliative care team also came in to see us. We talked about all of the changes that have been made, and about Benjamin’s shallow breathing and high pulse last night. They asked me to think about intubation. They said that while they don’t think it is at all necessary right now, I should consider how I want it handled if it is proposed. Well then. How exactly do I do that?
Benjamin received his platelet transfusion, and before our nurse started his red blood transfusion, she gave him Tylenol to decrease another rising temperature. He tried to take the liquid Tylenol orally, but he vomited immediately afterward. He asked for the pill form right away and kept it down. He is a total champ. You’re doing such a good job, buddy. You’re doing everything right.
After Benjamin vomited, he had a nice window of time during which he was much more himself again. I saw sparkle. He was doing things on his own that he hadn’t been doing in a few days, even picking on the nurses again. I decided I didn’t believe Dr. Wishnew. Benjamin was feeling better and that’s what I believed.
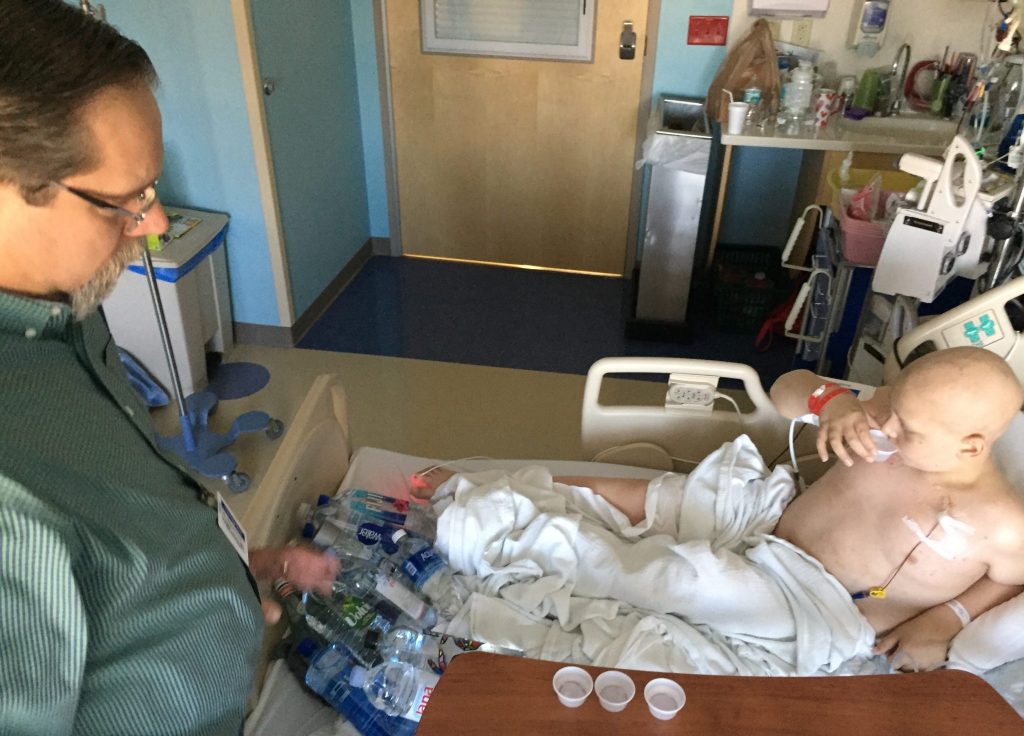
Benjamin was thirsty today. Maybe it’s because his veins are dehydrated, but I took it as an encouraging sign that he knew what he needed. Benjamin asked Michael to bring him some more bottled water, and in true daddy fashion, Michael brought seventeen different varieties. We were laughing and conducting a double blind water taste test when Dr. Wishnew and Shari walked back into the room. Dr. Oshrine was right behind them. As soon as I saw Dr. Oshrine’s face my stomach plummeted again. When they asked us to step out of the room, I wasn’t sure if I could walk to the door. Our nurse stayed with Benjamin. I had no choice. Stand up straight.
Michael and I were taken into a closed room and asked to sit down. The three practitioners began the conversation about what they called the elephant in the room. Benjamin’s condition has declined to the point where they feel that their decisions should be led by his comfort rather than a cure. The NIH trial is not entirely off the table, but Benjamin’s “clinical performance standards” (diminished lung capacity, organ disease) are making him a borderline candidate at best. There is still time for this round of chemotherapy to be effective. But every time we try and buy time with chemotherapy, we are potentially making his disease more resistant. They feel that his comfort and quality of life should be prioritized now.
We talked about all of the items we addressed in our email to Dr. Oshrine–the possibility of revisiting the trial at CHOP, doing another flow cytometry on Benjamin’s blood here to know where we stand, and introducing the idea of a PD1 inhibitor as potential therapy. He was open minded on every point, but was careful not to portray any false optimism. If we try the PD1 inhibitor, he thinks we should expect symptom relief, not curative therapy–and that’s a guess, because there is no experience with the drug in pediatric leukemia. The only evidence based bridge to transplant is the clinical trial, which would require a restoration of Benjamin’s clinical performance, and enough time bought with chemotherapy to get us there. They made this bridge feel very far away.
The room was spinning around me. Stand up straight. Michael took over the meeting when the practitioners were finished. He was somehow clear and controlled, laying out our priorities as he saw them. We have to find relief for Benjamin’s organs. We have to find a way to reduce their infiltration and ease the pressure on Benjamin’s lungs. The doctors said they will try as long as we ask them to. When I asked them what they needed from us, they said they joined us in hope, but they needed us to be thinking of contingency plans. If Benjamin’s condition declines, we need to be prepared. I could not look anyone in the eye. I needed to leave. I needed to get back to Benjamin.
After I emptied my stomach, we spent the remainder of the afternoon trying to make Benjamin happy. When he needed to rest, we sat with him, and I held his hand. We’ve been holding hands so much lately. It’s such an honor to be able to bring him comfort. Michael and I are completely united in hope. We refuse to give up. Benjamin felt better today than he did yesterday, and tomorrow he could wake up feeling better still. This round of chemo could still achieve its desired effect. We have no idea what each day will bring, but we are present for Benjamin and we will trust our instincts. We will stand up straight. He has shown us how.
Banyan stayed home for one more night tonight, nursing a lingering cough. He will join us tomorrow. Michael talked with him when he came home from the hospital and explained what the doctors told us. He shares our hope and was so sad not to be able to be with his brother these last few days. I am so proud of him I could explode.
Benjamin is sleeping soundly now, holding my hand. His fever has returned and his pulse is elevated, but his nurses have given Tylenol, and another port culture has been taken. He has received his chemotherapy for the night and his TPN has started its constant drip into his veins. His improved formula is on board. Everything is being managed well and his pain is under control.
Before Michael left, we started dreaming up our next camping trip with Benjamin. We wanted to paint a beautiful picture for him as he fell asleep, and for ourselves, too. Through pain and discomfort, through tubes and beeps, through his oxygen mask, Benjamin said so sweetly, “Let’s see. Where should we go?” Anywhere, love. We will follow you. We will be there with you every step of the way.
oh Mama. My heart aches for you. You have carried yourself so uprightly through these 760 days and I will pray for the continued strength you need to persevere one more, and then another, and another. Praying for a breakthrough that will bring you thousands more tomorrows with your boy. xoxoxoxo
17 different varieties of water ❤ Today will be better.
I join you in deep abiding hope. Absolutely.
I am sending continued hope and so much love. ❤️❤️
Joining in hope. Sending love.
Standing with you, united in hope.
I am not very good with words…but this post will not let me stay silent. Just wanted to let y’all know we are reading everyday and sending healing thoughts and energy your way. Praying his organs get some relief and he starts felling better. I am in awe of your family, and your strong brave boy.
Standing up straight sending hope and love ❤️
Always in our thoughts and prayers. Charlie Moody and family.
What a wonderful mother you are….I’m so proud if you, and so want to take your hurt away. Prayer and love….
God is pleased with his brave, brave
family,,,,
Never give up ….
I Believe……❤️
“You’re doing such a good job, buddy. You’re doing everything right.”
And I unite with you in hope.
Holding you up from here.
Hope and comfort to your boy and family,
❤
Benjamin the Brave! Give him a hug. We continue to pray for healing.
Laura, sounds to me like you are doing everything right. I am struck by the grace and elegance you write with daily. God has given your son the best gift… you as his mother. Praying for you all and for continued hope.
Joining you in hope and sending so much love. You are all doing everything right.
Hope is the thing with feathers that perches in the soul…Benjamin is your littlest bird, and you are his wonderfullest, bravest, strongest mama, period. Our hopes are right there with yours!
Our hearts and prayers are with you constantly. You are the example for us to follow as the best mother I know.
My heart is also acheing for you all. You all are a child of God, continue to stand up straight. Benjamin shows us all how to do that with his mighty strength. Sending Love and Prays for relief and healing.
praying and sending our love….so many thoughts and so many prayers….God Bless…
Every day I read every word. I am with you and your family. Every day is full of hope and love….❤
What a remarkable family! You stand united in hope, love, prayer and strength! Benjamin knows you are all there for him, he helps you stand tall! I pray for his relief….and healing….and your continued strength and love for your boy…..your brave boy!
You are making all the right choices. Please tell Benji we are thinking of him each and every day. I too BELIEVE!
❤️❤️❤️
Sending love and hope your way.
So many beautiful words from your friends and family on here. I’ll just agree with them through my tears and have absolute hope in Jesus’ mighty name! May god fill you and Michael with peace that passes all understanding and joy in the hope that is Benjis healing. . here on earth!!!
Oh Laura, even after years of serving as a hospice chaplain, I am learning so much from Benjamin, and the love and commitment of your family. So much beauty in the midst of pain and struggle. Sheer truth and transparent hope. The blessings you all have showered on so many people are immeasurable. I am filled with love and respect for you and your devotion and fierce attachment to your children. Sending warm extended hugs. I love you.
Gavin is keeping our church well informed and so many of us are praying for Benji, and for you and Michael and Banyan. The thing that brings me comfort in the midst of my tears is that in light of your obvious and incredible love for your precious son, is my knowledge that the Lord loves him infinitely more and is with Benji each and every second. Shalom
So much love to you all. Today and every day. You are a warrior mother and I am astounded each and every day at your bravery, optimism, and strength.
I am sending you love love love, all of you. Love, hope, healing and light. And most of all, extra love.
Sending all the love I have to give to all of you.
Constantly hoping, constantly praying, constantly sending love….<3
My heart aches for you all. I admire your strength and stand up straight with you in hope. All my love..
In tears reading this and my heart breaks for all you are going through. It is such a helpless feeling to want so badly to be able to do something and to know there aren’t even words that exist that could offer enough comfort. Know that you are in the hearts of so many and we are all praying and support and share your hope! Love to you all, and visions of complete healing and recovery for Benjamin the Brave!♡♡♡
I am a client of Michaels. I have been reading your posts for a while. I am so inspired by your love, knowledge and family. I am sending healing thoughts your way as you all journey through this difficult highway of life.
Standing strong with all of you. Much love.
Sending love and prayers….I am standing up straight with you today!
Laura, I don’t know what to say. You are the strongest person I know. You’re family is so beautiful in every way. A beautiful warrior family.
Every golden healing vibe I can muster is headed your way. Love to you all.
Standing with you in hope, knowing how precious each moment with Benji is and how fierce the desire for each moment to come
My prayers are with you everyday. I will not give up hope. There is nothing too hard for God. I love you all so much.
Every day we pray, send our love, and hope.
Your entire community is standing with Benji & your family! I pray for him daily!
I am praying so hard for all of you! Healing and hope and peace….
My heart is so heavy hearing this report, and yet I am so inspired and buoyed by your faith and hope and optimism. Wishing your amazing child renewed health and hope, and that all the care he’s receiving is successful beyond your wildest expectations. Peace and comfort and courage to the whole family as you walk this challenging path. We are all rooting for you!
Sending all the prayers and strength in my heart!! May the love we are all sending help hold you up straight through this!
Standing in spirit with you, beautiful Mama!!! My heart aches reading this post but it is your strength and the strength of your beautiful boy that is so very awe inspiring. Praying for your continued strength and courage every step of this amazing journey you are on. Praying for complete healing for Benjamin and relief from his pain. You are in my heart, my thoughts and my prayers!!
Joining you in hope. Sending love and healing to this amazing strong boy
We are thinking and praying for you all!
posted on my network and sending Benji as much love as I and they can muster.
Gilkey family- your strength is an inspiration. Your love for your sons so overwhelming beautiful. I pray that God may guide you in the direction best for you whatever that may be or lookilke. Benji is such an amazingly strong warrior with an unbeatable attitude. I’m so blessed that you are sharing his journey with us.
Standing up in HOPE and Love.
SENDING LOTS OF LOVE
XOXOXO
XOXOXO
XOXOXO
Sending much love to your beautiful boy, to you and your family, all the way from the north of Argentina to Sarasota.
Our family sends you all the love and healing we have to give.
Tell Benjamin that we follow his journey daily and that he is in our thoughts and prayers every day. With much love, The Cubillos family.
Sending hope and prayers your way. Stay strong and stand straight for Benji. Love and light,
The Sparkmans
Praying..I also feel hope and possibilities for Benji. Please God hold this family and give them everything that they need. They are the best of the best.
Hope, prayers, and strength sent to all of you. Your heart and instincts will guide you now. Peace, light, and love to all of you. You are all an inspiration, especially Benji❤
Laura, I just finished reading your post from 1/30 (that Andrea had shared, asking for prayers). I didn’t realize the full journey you and Mike have been on with Benjamin. My heart is heavy with all the information I just read; I am still absorbing all of it. Dan and I are joining you in hope; we will pray for healing for Benjamin and strength and for all of you .
Praying praying praying ❤️
Love and light and healing energy. You’re all so strong and I’m so proud from afar. You are an incredible family.
Sending prayers for healing and strength for you all.
Sending love and much hope to all of your Laura. <3
Sending so much love and hope from The Freeman family xo
My momma heart aches so hard with you for our Benjamin the Brave, Benjamin the Blessed, and Benjamin the Beautiful. I have no words, but know that you are surrounded by love and light through this newest darkness. Where shall you go indeed! Onward. So much love, we are out here for you. ❤️
Laura, I so wish there was something I could say or do. I wish I could shoulder a part of the burden of fear or that I knew of some miracle solution. You are one of the tallest standing women I know. Benji is full of light and love, and he is surrounded by so many prisms of light. I am sending you so much hope. I look forward to hearing all about this amazing camping trip. Let it be.
Your village is here with you every step of the way. So much love, prayer, and hope being sent your way to help you stand taller. Xoxo
Standing with you. Sending so much love and hope. Xoxo
We are standing with you and sending you love. Prayers going up.
You are an amazing, strong mother and family. I am
in awe of your strength and Benji’s courage. Stay strong
and keep believing. Stand tall and proud Gilkey
family.
Benji is such a delightful young boy. He always smiles and brightens your day. He is so strong which he definitely gets from his very strong loving parents. The few seasons we got to hang out together at the baseball fields were wonderful! Aiden would love to play with Benji again. Sending lots of love and prayers. The Zengel family
Sending love ❤️ and prayers
Praying for you and your family!
Dear Laura and fsmily,
Sending you love, hope, strength and prayers.
We have never met Benji but love him nonetheless! Praying for his treatment to heal him very soon and we hope for continued strength for you and Mike…you are both amazing!
You all are so embedded in my thoughts every day. I am sending all the hope and strength and healing that I have. And love, so much love. Benji is one incredible boy and the Gilkeys are an incredible family!
Stand up straight, mama! I will kneel, in prayer, asking that you and your lovely family can continue to find strength and healing through these many twists and turns. You all are so loved!!!!! ❤️❤️❤️❤️
Stand up straight, mama! I will kneel, in prayer, asking that you and your lovely family can continue to find strength and healing through these many twists and turns. You all are so loved!!!!! ❤️❤️❤️❤️
You’re in my thoughts and prayers and I’m sending you and the entire family so much love.
Standing with you.
You are an inspiration beyond inspirations.
Holding space of love & serenity for your entire family.
Sending love and prayers for Benji and his family. Your blog brought back many memories from when our son was at All Children’s and our day was all about his number count. One day when things were not looking good I asked the doctor how I was suppose to handle it and she told me we were going to take it one day at a time. That helped me then and its a lesson I carry with me now everyday. I learned so many things from that journey: love, hope, faith and most important – to let other help me. I am praying for Benji and his miracle. I saw so many when I was there.
Fondly, Deb Lombard (Southside dance teacher)
Dear Old Friend,
I\’m just now finding this love song for your family that you\’ve been writing for 760 days, a natural extension of the joy and devotion you have unleashed on the world your whole life. Of the comforts the doctors desire for Benjamin, they have to know, if they haven\’t acknowledged it aloud, that the greatest comforts come from all that you and Michael have been doing. There\’s little doubt, in the very few posts I\’ve been just starting to read, that Benjamin is cognizant of his potential peril and is also wholly comforted, knowing that whatever he does, wherever he goes, whatever his frailties may be at the moment, there\’s no reason to fear, for his family is backing him up with everything they\’ve got. That message is transcendent, resonant into eternity, and more powerful than any illness. I would posit that the brilliant sparkle you see in that little boy started as a reflection of what your whole family has poured into him, but it\’s clear that at some point he took control and magnified it as his own unique expression of love back at ya. That\’s just what wonderful children do!
Praying for the blessings of Benjamin the Brave\’s complete healing, your strength to keep standing up straight, great family camping, and hearty belly laughs.
We are praying for you Gilkey family. Thank you for sharing this unbelievable journey. Your strength is so inspiring. We love you Benji!!
Walking with you, abiding with you, standing up with you. Sending prayers for Benjamin’s healing, and immense love you and your beautiful family. Always and with every breath.
Praying for your family at this moment. You are amazing, he is so so brave!!
What a story! Your family is so brave in this fight! Prayers to all of you! :::sending sunshine::::
I join you in love and light and absolute hope. LOVE.
There are no words. I send you so much hope and love….
I have been deeply noved, inspired and more open to this world around me. As a Mother I am affirming my belief that love will always be the answer. It heals and brings people together in ways we never thought possible. This is a truly a lesson for all of us. Your strength is my strength your sorrow is my sorrow For You Are Not Alone