Benjamin’s procedures have all been completed safely. He slept comfortably through almost everything. Now, we wait, as we have done so many times before.
I stayed awake through Benjamin’s first platelet transfusion at 2am, then we both slept as late as we possibly could. I peeked at his labs during shift change. They held steady with a white count of 5,000 and 84% blasts. Benji is profoundly neutropenic with an absolute neutrophil count (ANC) of just 40. The late night platelet boost brought him up to 19,000. He would get another transfusion before the events of the day.
A physician from the pain team came to see us while Benjamin slept. She had a student with her, and she wanted the student to feel Benjamin’s spleen. The student seemed nervous, like she didn’t want to touch him. I didn’t want her to either. I know this is how physicians learn, but it stings that my son is the subject of lessons and textbooks. I was glad when they left.
The first words out of Benjamin’s mouth today were urgent: “Bucket! Bucket!” Our resident nurse had used a predrawn saline flush, not expecting his aversion to be stronger than sleep. Within the first minute of wakefulness he was vomiting. Afterward, he seemed to feel much better. Michael arrived for the day, and we started talking about the feeding tube and when it might come out. We told Benjamin that before it did, we would probably use it to get him some nutrition. He asked what they would put in it. We told him it would probably be kind of like a smoothie. He nodded and thought that would be a good idea. He was also asking for water. Both of these were great signs, in my opinion.
The window of feeling well was short-lived. Just as the surgery transport tech came to take us down, Benjamin vomited again. He asked to use the bathroom and finished vomiting while simultaneously producing very dark stool. I’m scared of what this CT scan might show, but we need the information. Clearly.
Our nurse hung a dose of Ativan on Benjamin’s IV pole to help him with nausea and ease his anxiety. We went downstairs and were greeted by our favorite Special Procedures nurse. We answered all of the routine questions and made sure everyone was on the same page with the lumbar puncture, triple intrathecal chemo, nasoduodenal tube placement and port reaccessing. The transfer of information from 7 South to SPU was seamless and impressive. We gave Benjamin as many choices as possible–which side of his face the tube would be taped to, when the nodes and oxygen would be placed in the operating room, and where he’d like to be when he woke up. We didn’t have to wait long before it was his turn. Michael kissed him goodbye, and I walked with him down the bright, familiar hallway.
Benjamin knew so many people in the operating room–the physician doing the procedure, the anesthesiologist, several nurses and two residents. They were all smiling when he walked in, and he reciprocated. As he was preparing himself to receive the propofol he became a little afraid, specifically about the tube placement. I watched him close his eyes gently and sink into himself, finding his peace, and settling into it. The fear left his face and left the room. He is so incredible. I kissed him goodbye and found Michael waiting for me.
We usually grab a bite to eat while we wait for the surgery pager to beep, but today, neither of us were hungry. My stomach was a wreck. We found a bench outside and enjoyed the sunshine and the breezy, gorgeous January day. We voiced our fears. I told him about a dream I’d had over the weekend. Benjamin was sitting in a chair on a dark stage, and he was being scanned. A buzzing blue light signaled every time the scan found a new cancer. It was oddly like the Sorting Hat scene from Harry Potter and the Sorcerer’s Stone, except that it was a total nightmare. We also voiced our hopes, together. We strengthen each other’s resolve.
We went back to the recovery room while Benjamin was still soundly sleeping. The tube was placed in Benjamin’s right nostril and loosely taped to his face, along with an oxygen cannula. It was kind of a shoddy tape job; when we went back to the room, our nurse removed the cannula and the tube came along with it, dislodging it by an inch or so. Fortunately the x-ray that was taken a few minutes later showed that the tube was securely placed in the duodenum. Our nurse mixed the contrast dye powder (called Gastroview, not kidding) with orange Gatorade and poured the solution into a clear bag, then hung it from Benjamin’s IV pole and ran it through the new pump. The liquid would run through Benjamin’s body for the next several hours.
Benjamin woke up a few times to urinate, or to look around the room, or adjust his position. But mostly, he slept through the discomforts of the day, and Michael and I were so thankful for it. When he first woke up, he was afraid. His eyes were wide and he said he thought he swallowed the tube. Michael and I assured him he hadn’t, and that it would just feel a little strange at first. We told him everything had gone perfectly in the procedure. He went back to sleep. He was sweating profusely all day long, soaking his pillow, blankets, clothing, everything. I believe this is because of the hydrocortisone that was added to his intrathecal chemo to tackle the blasts they found last week.
The nurses were monitoring Benjamin’s vital signs closely, using oxygen when they needed to. At one point a nurse put a blood pressure cuff on the same leg that Benjamin’s oxygen monitor was on. His pulse dropped dramatically on the machine and I panicked. As soon as I realized what happened I was so relieved I couldn’t stop the release of tears. Everything just kind of came at me in that moment.
The contrast took a lot longer than it should have because the pump kept stopping to beep at us. It is designed for thicker, heavier substances like nutrition supplements, and the weight of the Gastroview wasn’t registering consistently. A six hour contrast window turned into seven and a half. Michael was planning on staying through the scan, but it was getting late, and he had to leave to be with Banyan, who’d spent the evening at a friend’s house. Before Michael left we ordered some delicious Thai takeout and had a makeshift date. We miss each other.
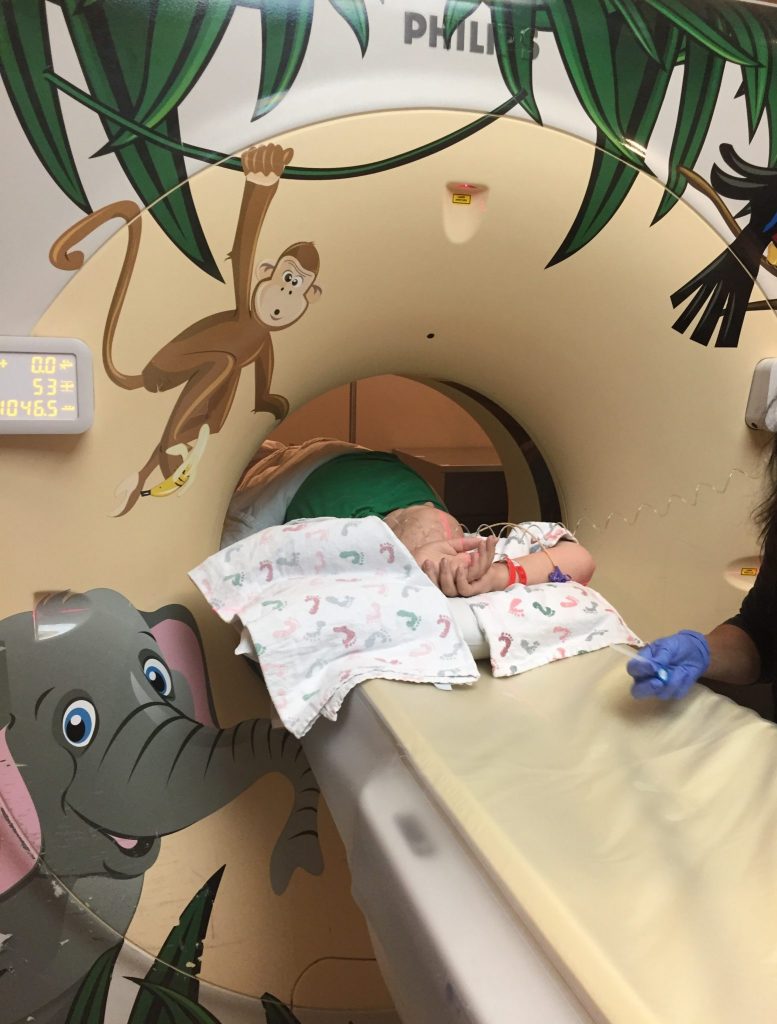
When the contrast was finished and had time to really absorb into Benjamin’s body, we were sent down to radiology. It was almost 11:30pm. A second nurse helped our nurse and me navigate the halls with Benjamin’s bed, pole, and pumps. The raspy radiology technician was very kind to Benjamin. We all helped slide him from his bed over to the CT scan bed. She injected a counterpart to the contrast through his port that would react with the Gastroview to illuminate everything. Then she went into her little room and spoke to him through a speaker. “Deep breath. You’re doin’ great honey. Just one more picture.” It was over quickly. We went back upstairs and settled into bed. It’s been a long day.
Tomorrow morning, our attending physician and nurse practitioner will review tonight’s scans with the radiology team. They should have results for us during midmorning rounds. I’m also hoping to learn what Benjamin’s cerebral spinal fluid looked like today, and possibly to touch base with NIH. But we are taking things one day, one breath, at a time. Nothing feels certain right now, except that Benjamin has handled everything that has been asked of him with bravery and grace, just like we expected he would. His courage gives us courage. His tenacity gives us hope. Tomorrow, we will do the best we can with what we have, and wrap him up with love.
❤
Thinking about you, Laura
Love and Prayers
I Believe….❤
And wrapping you all up in love, too
Hoping you get an ‘exhale’ with the day’s results
You have all taught Benji so much about how to take each different feeling, sensation, uncomfortableness and let him know the best way to help him through it. Keep on that path. Much love ❤️
Think of you all each and every day.
I am wrapping all of you up with love and prayers
Once again, Benjamin proves to be an exceptional person in the face of challenges that would shut many of us down. Hopeful for positive answers today.
Bravery, courage, grace, and tenacity…..Benjamin, you are incredible. I hope the days become less difficult and the path becomes clearer. Thinking of you always. xoxo
Wrapping all of you with much Love and Prayers.
He is such an amazing boy. Sending love ❤
The Singers are sending you all our love, prayers, and healing thoughts. Benjie is an amazing young man! As the old saying goes, That apple did not fall from the tree! You are an inspiration to us all.
I love you all so so much. <2
Praying for answers and relief. Benji is fighting so hard. Wow! God bless and protect you all. All4!
All our love & prayers
{{{❤}}}
Sending you healing thoughts and prayers.