Today was a hard day. I was determined to meet its challenges head on. I wanted to help Benjamin feel better and smooth his path toward healing. There were moments that threatened to undo me and I was not having it. No thank you, fear. I have no time for you now.
The first thing I saw this morning was our nurse practitioner’s face. She was giving Benjamin an exam as he slept. I jumped up to look at the morning labs. Benjamin’s white blood cell count was back up again, higher than it’s been in several days. My heart sank, and I steadied myself. It doesn’t look like Sunday was a fluke after all. And 89% of the white cells counted were leukemic.
I don’t know what this will mean, or if the coming days will show anything different. But I felt this fire in my belly to do something. I am so tired of waiting. I used the remainder of Benjamin’s morning sleep to research. I searched things I’d searched a hundred times and things I’d never searched before. I used new combinations and new angles. Underlying all of this is Benjamin’s CMMRD, and everything needs to be examined through that rare and complicated lens.
I composed my thoughts and emailed Dr. Oshrine. I know he is keeping an eye on Benjamin’s labs and thinking about possible alternatives to this interim therapy. I told him that I am also concerned that as his leukemia progresses, Benjamin’s T-Cells may be less effective for use in CAR-T therapy than they were when we collected the first time. I’d like to petition NIH again to consider using the cells we already have, both in the interest of time and efficacy. Finally, I said what I’ve been holding back for days now: I’d like to have a conversation about how we might facilitate the compassionate use of a PD1 inhibitor if the NIH study falls through. We can do so with the guidance of the physicians I’ve found in Toronto and Stanford. I don’t want us to need this option, but I want it to be available if we do.
Benjamin experienced vomiting and diarrhea within just a few minutes of waking up this morning. I requested his first dose of Marinol. He was not happy with me. He thought, once again, that the pills would make him vomit, but he dutifully took them and we moved on. I was determined to create an uplifting environment for him today, with music, aromatherapy, art and schoolwork. We had to cut the art short, and we never made it to the schoolwork. An hour or so after taking the Marinol, Benjamin vomited again. I told you, he said. I knew the Marinol wasn’t making Benjamin vomit, but it clearly wasn’t working either. The trifecta of Kytril, Scopolamine and Marinol is not enough anymore. Time for a change.
I texted our nurse practitioner and requested a consult with gastroenterology. Seconds later, she walked in the room with the attending oncologist, charge nurse, nurse, trainee, and patient care technician. They’d been outside for morning rounds, and apparently they were thinking along the same lines. We have to get to the bottom of what’s going on in Benjamin’s belly. I know that Benjamin’s leukemia, enlarged spleen, lack of food and cocktail of medicines is probably responsible for his continued pain and nausea. But any other explanation that can be ruled out must be ruled out.
We can’t do a colonoscopy or endoscopy right now, but we can do a CT scan. So, tomorrow while Benjamin is under anesthesia for his lumbar puncture, he will have a nasoduodenal feeding tube placed. This will allow him to have the proper amount of contrast dye put into his system without him having to try and ingest it and keep it down. Benjamin’s port will also be reaccessed while he is asleep. Once he wakes from the procedure, he will finish receiving the contrast, then we’ll head to radiology for the CT scan. The tube can be removed at bedside, but I don’t think that will happen until Benji is ready to eat on his own again. It’s been eight days since he’s had a proper meal.
As soon as it was explained to Benjamin that he would wake up tomorrow afternoon with a tube in his nose, his whole spirit fell. He was nervous and sad and distant. It was so painful to watch. I tried to explain that the alternative is drinking a ton of yucky tasting stuff. This helped a little, but he still seemed so resigned. Here’s another really hard thing he’s being asked to do. He’ll do it with grace and bravery. But the hard things keep coming. It’s exhausting sometimes.
While Benjamin slept, the sweet physician from palliative care came to visit. We talked about ways to adjust Benjamin’s medications to try and tackle his nausea from another angle. The doctor said that nausea was just as unacceptable as pain for a little guy. I like this doctor a lot. We decided to eliminate the Marinol and replace it with Phenergan. I told him I would make the change after Benjamin woke up and agreed to it.
Benjamin’s nap was a long one. Kathy and Gana came for a visit just moments after he woke up. He wasnt feeling well at all and just wanted to lie in bed and watch television. They understood. I wanted to give him the Phenargan but every time I mentioned it–or anything else that might make him feel better–he held up his hand to stop me. It is so important to me that he maintains some agency with these things, but we have to strike a balance.
As the workday came to a close we were visited by our nurse practitioner and the attending physician. They had coordinated everything with surgery, gastroenterology and radiology, and Benjamin is all set for tomorrow. The radiology team directed our team on how to schedule the contrast so that Benjamin’s colon, specifically where his polyps are, will be best illuminated. Benjamin will also have a special pump for the tube that regulates what goes into it. This makes sense of course; his normal pump only controls what goes into his port. But hearing this detail felt like another punch in the stomach. Essentially this is a feeding tube. That’s what’s happening tomorrow.
Michael and Banyan came up as soon as work and school were over. Benjamin didn’t feel any better when they were here. We were able to get him bathed and comfortable. We were hoping to spark some interest in food, but we had no luck. I’m grateful for the intervention that is happening tomorrow. I’m grateful for the chemotherapy that will keep his central nervous system safe. I’m grateful to be able to get a different look at Benjamin’s gastrointestinal tract. And if he still doesn’t eat, I’ll be grateful for another way to get him some nutrition.
Today was a hard day, and tomorrow will be a hard day. But we can do hard things. Benjamin shows us how. We will help make tomorrow as comfortable as possible for him, and hope that the right answers will follow.
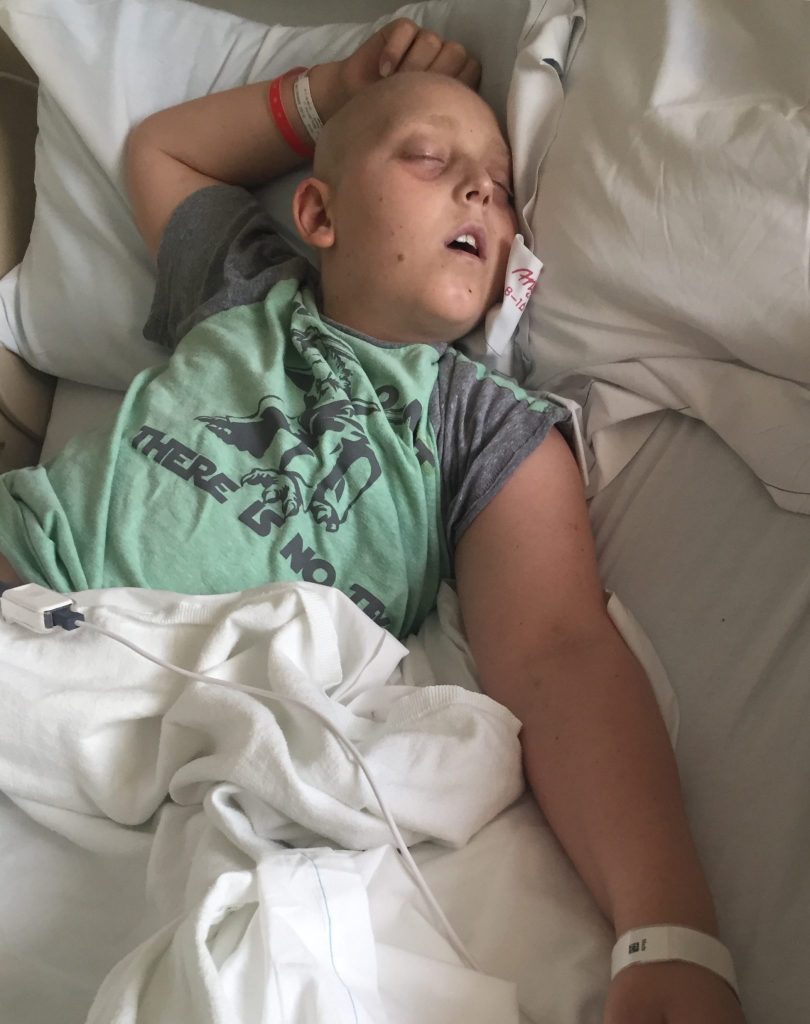
I walk beside you. You fly with brave wings. Isn’t it amazing what we can do! Who would have thought! Love,
Marcy
❤
Praying-praying-praying!
I am so glad to hear you have some support in finding new ways to address the nausea, and hope the addition of nutrition will help alleviate it, and build his strength and spirit. You are all so, so brave. I hope today brings new hope, new healing and we send you love to fortify your strength, courage, and wisdom –
https://www.youtube.com/watch?v=WtSFa9I6fh8
You, Laura are a powerful force! This path you are on with your family is hard but what a champion Benji is.
With you and your tribe…..
Prayers and Love…….
I Believe….❤
Tough day….prayerful for relief and good outcomes Wednesday.
May God bless you and keep you and give you strength. We are praying for you as a church and today will be praying in unison for you.
Love and Prayers to continue.
Oh my gosh so many hard things to face. Lord let his miracle prevail here and now!!!! HERE AND NOW!
My Thought and Prayers are with you always… giving you some extra strength. Love You!
There is one Love and you both are bathed in it, enveloped in healing light. Untouched. No pain, no fear… only wellness, strength, and joy. As you walk through this narrow place you both are being squeezed, and still you will come out the other side renewed. Benji is doing such hard things, and his bravery will benefit so many. One day soon we\\\\\\\\\\\\\\\’re going to get to change his title from Benjamin the Brave to Benjamin the Breakthrough. His way is made with each act of gentle bravery, and his determination and courage will sustain him now with a heroic story he can tell forever. Thank you, Benji and Laura. We all love you so much. Sarah and the Checcone family
There is one Love and you both are bathed in it, enveloped in healing light. Untouched. No pain, no fear… only wellness, strength, and joy. As you walk through this narrow place you both are being squeezed, and still you will come out the other side renewed. Benji is doing such hard things, and his bravery will benefit so many. One day soon we’re going to get to change his title from Benjamin the Brave to Benjamin the Breakthrough. His way is made with each act of gentle bravery, and his determination and courage will sustain him now with a heroic story he can tell forever. Thank you, Benji and Laura. We all love you so much. Sarah and the Checcone family