Since Benjamin’s diagnosis, we have asked for guidance to make decisions for his highest good. Today we were guided in a direction we did not expect, but one that could not have been more clear. We are staying on the seventh floor.
Last night, Benjamin had a high fever and rapid pulse, and he was shaking. He experienced more occult blood in his stool. He asked for solace in a warm bath, and I held his head against my arm to keep him from falling. We tried giving him Tylenol by mouth to prepare for a potential transfer to hospice care at home (intravenous Tylenol is very hard to come by). He swallowed the pills perfectly, and kept them down; but they had absolutely no effect. We used cold washcloths and his fever broke naturally. We slept.
This morning during rounds we learned that both transfusions Benjamin received yesterday disappeared completely. His platelets and hemoglobin were even lower today. The products aren’t being absorbed. This is partly because of Benji’s recent fevers, partly because of his gastrointestinal bleeding, and mostly because of his volume of leukemia. We decided to schedule intravenous Tylenol around the clock to try and stay ahead of his fevers. We also decided to give Benjamin a double volume of platelets today, and withhold the packed red cells. They are no longer offering Benjamin the benefit they once did. He has had his last red blood transfusion.
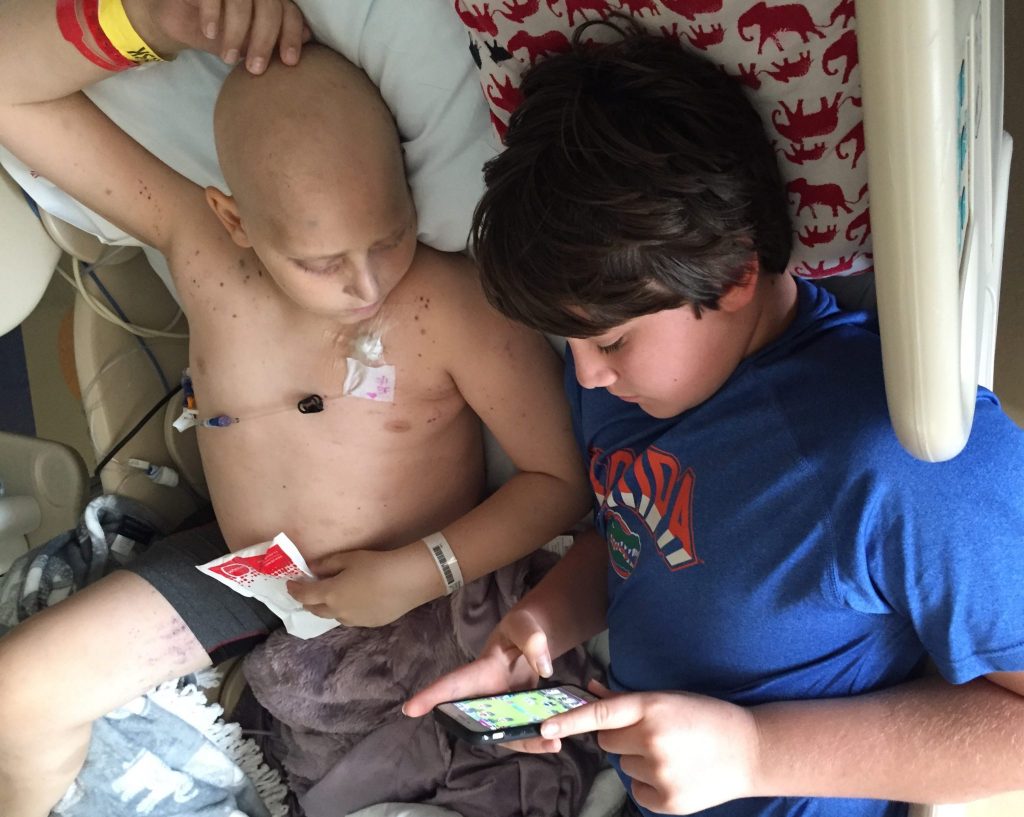
Benji asked Banyan to lie in bed with him this morning, during what would be his only window of wakeful alertness today. They played games and enjoyed being next to each other. They shared donuts that Kathy and Gana delivered per Benji’s request. Banyan has been so beautifully in tune with his brother’s needs. He holds his hand when he is uncomfortable and he doesn’t get his feelings hurt when Benji needs space. He helps him to and from the bathtub and is the first to fetch fresh ice for Benji’s root beer. I’ve told Banyan many times that he doesn’t have to stay in the room if he’s uncomfortable, but he has said firmly that he isn’t going anywhere.
So, Banyan was here when the hospice nurses from Sarasota came to explain their services. We were joined by the Palliative Care physician, our nurse practitioner Shari, and Marris, our wonderful nurse. We all worked together to come up with compromises that might make a transfer feasible. We’d agree to platelets every other day, we’d eliminate Benji’s antibiotic, we’d replace Narcan with Benadryl for itching–things like that. I was feeling ready to go home. All of our questions were answered except one.
I asked Shari and one of the hospice nurses to step outside with me and find a private room. I needed to know what would happen at home at the time of death. We have specific requests that we want to be sure are addressed. While the process was explained, we were joined by the other hospice nurse, the attending oncologist, and the Palliative Care physician, who wore a disappointed expression. He had just spoken with the hospice physician from Sarasota. The hospice physician was concerned that they wouldn’t be able to meet Benjamin’s needs. With platelets that are consistently so depleted, bleeding becomes a serious risk. For the first time, it was explained to me that Benjamin’s recent occult blood and lack of platelets could result in a gastrointestinal hemorrhage.
This complicated our decision considerably. On one hand, Benjamin has had so few platelets for such a long time. He has never had an issue with excessive bleeding and I don’t believe it will happen now. On the other hand, should a hemorrhage occur at home, it would be much more traumatic than at the hospital. The Palliative Care physician was thinking of Banyan. Here, we can get platelets whenever we need them, day or night. I needed to talk to Michael.
As if he could feel my indecision, Michael walked into the closed room next. He said that Benjamin had been asking for me. I asked the team to go over with Michael what we’d discussed, and I ran back to our room, where Benji was trying to navigate his way to the bathtub with help from the nurses. He was in serious pain.
Our conversation with Benjamin about his transition is evolving. I find myself talking to him during his baths, when his body finds sweet relief and his head is resting against me. I told him today that no matter how much his body hurts, the energy that lives inside him cannot be hurt. It is as bright as a star. It was here before he was born and it will be here after he dies. I told him that he has been so brave, and has worked so hard. It is okay if he wants to keep working and we will work as long as he wants to. But it is also okay to let go. Sometimes letting go is the bravest thing.
Benjamin returned to bed and experienced the worse pain I’ve ever seen. He was arching his back and screaming, and his eyes were wide and afraid. His cries were audible in the hallway, through the sound absorbing walls. Benji pressed his button and we requested a nurse bolus of Dilaudid as well as an increase in his continuous dose. We also requested Ativan to ease Benjamin’s anxiety. Our nurse was in our room within seconds to make the changes. I thought about trying to navigate such a situation at home, where we would have had to call a nurse to come and increase the dose, possibly waiting an hour or more. The experience solidified my decision.
Michael walked in while Benji was in pain and came to the same conclusion. We told the hospice team that we needed to talk with Benjamin to be sure, and that we would get back to them by tomorrow morning. During Benji’s next trip to the bathtub we asked him if he still wanted to go home, or if he would be comfortable here. He truly did not care what we were asking him. He just wanted to be free from pain. Our decision was clear. Only one of our options could provide platelets day or night and respond to his pain needs on demand. We will stay here, on 7 South, with this family who has wrapped us up in their care.
Today was another intense roller coaster. I can only imagine how Benjamin feels. I am grateful for the clarity that helped us make the difficult decision to stay here, with the nurses we love and the platelets and pain response we need. Benjamin has done everything that has been asked of him for more than two years. So much bravery. So many hard things. He deserves a peaceful passage, and we will do whatever we can to help this happen. Peace is our clear intention now.
Laura:
l feel certain you have made the right decision.
Love,
Sonia
I am praying for your family I am praying for your heart your pain. I am praying for Bengies hurts his suffering and his pain. You guys are in my heart
I am praying for Peace and sending love and light to Benji and each of you.
Praying for peace.
Laura, Michael, your courage and wisdom at this time amaze us. I know Benji is everything right now but please remember to take care of each other as well. We’re thinking of you and the boys all the time. Peace and love to you all.
Holding you all in my heart and sending love and peace.
Grateful for the choice, for the constant courage shown by you and Michael, and for steadfast Banyan. Dear God, comfort Benji.
Praying throughout the day and into the night for your Benjamin. Thanking God for Benjamin.
Holding all of you in my heart.
I will continue to pray for you all. Your own bravery and ability to meet Benji’s needs is inspiring. Please remember to take care of yourself as well. Much love from Alabama. I wish there was something I could do to help you.
you are home (where your heart is). envisioning peaceful, loving energy surrounding you day and night.
I wish nothing but peace for you during this transition.
Praying for peace and comfort for the entire family!
Sending our love and hope for Benji’s comfort and peaceful passage. You are an amazing family, and Banyan – what an amazing brother. We love you guys. Xoxo
❤
Constant prayers. Constant Peace. Constant Love. <3
Just thinning of what Carmela says, that it is not where you give birth, but how. All my love.
Just thinking of what Carmela says, that it is not where you give birth, but how. All my love.
Gathered all the Pastors at the church this week for a time of prayer for Benji and all of you. May the peace of God be real in your lives.
We continue to pray for peace, strength and guidance.
Peace
Honor ….❤️
You are in my heart and I am praying with everything I have for peace for your beautiful family…
I believe your family is where they need to be. Hospice is a wonderful option but the needs of Benji are being met so beautifully where he is and that is a comfort for you, Michael and Banyan. You’re doing such a wonderful caring plan for your son. ❤❤❤
You are a wonderful mama.
You are all so brave – I know the Lord is guiding you in your decisions, I am praying for each of you
We are with you in prayers constantly. May you and your family truly feel the love and peace from God. Hold tight, this place is not our home.
Revelation 21:3-4 Behlold, the dwelling of God is with men. He will dwell with them, and they shall be his people, and God himself will be with them, he will wipe away every tear from their eyes, and death shall be no more, neither shall there be mourning nor crying nor pain any more, for the former things have passed away.
It is possible to have more than one home, and it sounds as if, with your love and the love of the caregivers around you, you have ask made a second one right where you are. I have been thinking a lot about Banyan. What a gift for him and Benji that he has the ability to be so present with his brother through this transition. The energy glows brightly inside all of you. Sending love and prayers.
Praying for peace for all of you. Sending you so much love ❤️
Praying for all of you through tears for you. Laura, you are making the best decisions for your whole family. No one could do more than you have. Love to all of you.
Holding you all up in prayers for peace and relief of pain.
Strong like the , Bandon stands for his brother. We send our love and prayers.
Praying for peace and comfort for you all and that Benji’s pain will be well controlled. Thinking of you all constantly. You’re making the best decisions for him. ❤
I know you all will make the best decisions just like you have been doing for last few years. Sending much Love and Prayers
These decisions are wrenching-holding you close and sending peace. ❤️❤️
May the Peace of the Lord be with you, Benji, Michael , and Banyon ALWAYS. All my love…..
I am praying for you all to find peace and light.
Praying for peace
Praying for peace and comfort for Benji and your entire family. My love is with you all.
Prayers for peace and strength! xo
Praying for comfort. Sending LOVE.
I wish for a peaceful passage for Benjamin. May Gods love surround all of you. Continued prayers.
We pray for you all daily. I pray today is as smooth as possible for all of yall. You all are all so brave.sending love and comfort your way.
Your amazing village has no bounds. You have described an incredible process of discernment and intuition. Thank you for sharing it. I affirm that your clarity is spirit led and I love you.
Praying for peace and comfort. Love you all with all my heart.
We sang for you this morning.
“Holy Spirit, You are welcome here
Come flood this place and fill the atmosphere
Your glory, God, is what our hearts long for
To be overcome by Your presence, Lord. ”
You show the power of parents’ love. Your family is filling my heart with love.
I haven’t met your family but your posts kept showing on some of my friends timelines so I started reading them. I am so sorry for what you all are going through. Despite all the pain you all must be in, your love, care and groundedness in tending to Benji’s needs is amazing. Benji is very blessed to be surrounded by such love from his family and community as he goes through such a challenging time. My tears and prayers go out to Benji and your family. God bless you all.
You are strong, you are making the absolute best decisions you possibly can in the circumstances you have. Stay strong, praying for you guys. Hugs and love from Michigan.
Laura – you are guided as you always have been – I pray for you , you and Benji – the profound Grace of yours and his spirit yields to peace and love ❤️ ❌⭕
Praying for peace. xo
You are all in my heart and thoughts ♡
Benjamin the Brave is surrounded by an equally brave family. Sending peace to you as you continue to make decisions that are right for your child. Bless you all.
Surrounded by love, near and far. That is the best way to journey. Praying for peace and comfort now and always. <3
An army of prayer warrior and caring friends…more than you can imagine, are following your journey every day.
Benjamin’s courage and that of his family is miraculous. The love that abounds amongst you is the only emotion that surpasses that courage.
My love and prayers,
Phil
Seems that this 7th Floor room Benjamin is in, visited so often by nearby family, accommodating to your living there with Benjamin, and surrounded by a surrogate medical family of competent and caring professionals, is a space that was made for you all to endure this trial. Your choice in discernment to stay or go seems very well grounded, hard though it is to let go of his old home. Working all angles so strategically to maximize his comfort to the ultimate conceivable degree is the best you can possibly do. Your strength seems limitless. May your heart be preserved and your strength remain throughout all that will come to pass.
Home is where the heart is, and for this journey, he may be home, where he is loved, as always, and comforted, as only he could be on the 7th Floor. God bless you and keep you present in grace for Benjamin, and bring you all through these transitions peacefully.
Your courage is amazing. I love you all so much. You are in my heart day and night. ❤
Laura,
I continue to lift Benjamin, you, Michael and Banyan up in prayer. What a beautiful relationship between brothers….Banyan is the perfect big brother:). May The Lord bless Benjamin with comfort and a peaceful homecoming. Thinking of your entire family and praying, praying, praying.
I am praying so hard for your family right now and will continue to do so. Seeing your sweet boys in this picture makes me laugh and cry at the same time. First, I live in Gainesville so my 9 year old son has plenty of gator shirts which I see your boys are big fans. Banyan and Benji are playing Clash Royale and no doubt discussing what “legendary” they should use in battle. This is also a favorite game of my sons. I can’t imagine what you are going thru but I am in awe of your grace and faith. Wishing and praying for much bravery, strength, healing and peace to you and your precious circle.
Sending you love and wishes and prayers for peace.
You and Michael are so strong, Benjamin is so strong, Banyan is so strong. The strength is love. I’m wishing a gentle journey for Benjamin, a release from his physical torture. I am so, so very sorry for his illness and what it has done to your family. Blessed be, Benjamin. Peace to you all.
I’m in awe of your strength and pray for you all daily. You made the right decision staying. I read your updates and prayed that you find these things out from hospice before making the move, clearly you have asked all the right questions. We brought my mom home under hospice care and night one they were unable to control her pain….it haunts me and I regret the decision to this day. Continued strength and prayers to you all….
love and compassion.
May the peace of Jesus, the peace beyond all understanding, fill Benji and each of you. I am praying lots for each of you. May Benji find freedom from fear & pain. May he find great comfort in knowing the depth of your love (and God’s love) for him. Sometimes, I see life as a pregnancy- we live in the womb. As death approaches, we move into that transitional phase of labor. It is difficult, but what awaits is a wonderful birth into eternal joy, peace, and love beyond anything anyone can begin to imagine. Love & Prayers to you.
Your courage and bravery continue to amaze me. ….sending love…
Still sending love and prayers yalls way. We love you all.
So sorry he is in this pain and that your family is facing this. Big hug. Thank you for sharing your journey. Sending love to Benji and all of you…
I am so sorry to hear about Benji’s struggle. May God give you strength and hold your family close. Much love to you all.
Praying for your entire family. Sending love, hugs, and positive thoughts.
You’ve made the right choice. We will continue to pray for peace and love, that when the time comes, he will make the transition peacefully with you and his family loving him as he returns home. God bless you, I am so very sorry your heart and his hurts so badly. May the angels bring you comfort and peace.
I don’t know you, and I only started reading your posts last week when a friend of mine began posting them on Facebook, but I just want you to know how moved I am by your experience and your beautiful, heartfelt writing. What a special family you have. I am so sorry for what you are going through and wishing you all peace.
Sending you peace and love. <3
Laura , I realize now that our physical paths have not actually crossed, but our common link is Sarah Culver. I am just sending you love, and light as you and your family walk through this.
Laura, Over the last few days that I\\\\\\\’ve read your posts, I have felt not only your desire for peace, but your passionate pursuit of it for Benji, Banyan, Michael, for yourself, for all who love you. Benji\\\\\\\’s not the only one doing everything right. Your presence, your vigilance, your commitment, your gratitude, your thoroughness, your resolve, your confidence in the decisions that must be made, and your spacious, luminesce trust throughout your marvelous boy\\\\\\\’s transitioning is so humbling, awe takes over and words fail. Love is a miracle if it\\\\\\\’s cared for, served, nurtured.. You and your family and your expression of that love are a living miracle. Our We are breathing, sending, pursuing peace for you all… peace in every cell, every breath, every thought… That is the truth about your boy. Peace… And not a stagnant peace – not for Benjamin the Brave…. a peace that protects and lifts and comforts, as fierce and unceasing as your love. Powerful, Unbroken, unstoppable. Just like his incredible mother. Sending so much love to you all. You are enveloped in peace with love.
Benji, your incredible strength & courage is beyond words. Sending never ending prayers and unconditional love to you and your family.
You and your mothering and your writing and your family (especially Benji!) are so inspiring, I’m so sorry for your pain and wish to send you so much love and peace <3
Thinking of Benjamin tonight.
What a priviledge it is to witness this sacred journey your family is undertaking Laura. Thank you for being generous in sharing. You have a gift of finding sweetness in such bitter circumstances. I imagine Benji finds comfort and safety in your presence. You are doing everything right. I pray that you and your family continue to find comfort and strength as you spend your last moments with your brave, beautiful, young Benji. May sweet memories light the path through the darkness. I am so sorry that you are having to walk this path. We will continue to fight this ugly monster Leukemia and always remember those who have worked so hard like your Benjamin. <3
Thinking of Benji and all of you tonight….
Praying for this to be easy for Benji. Praying for no pain, just peace.
Hearts and hugs to you all.
Sending all our Angels to surround Bengi and your family with hugs. Lifting all of your family up in prayer. Much Love from a family who has been there.
RIP Brave little soul. May God be with you and comfort the family. May the angels bring you peace.